Varicose Veins & Treatment Options
Ready to take the next step?
Hear from Dr. Costantino
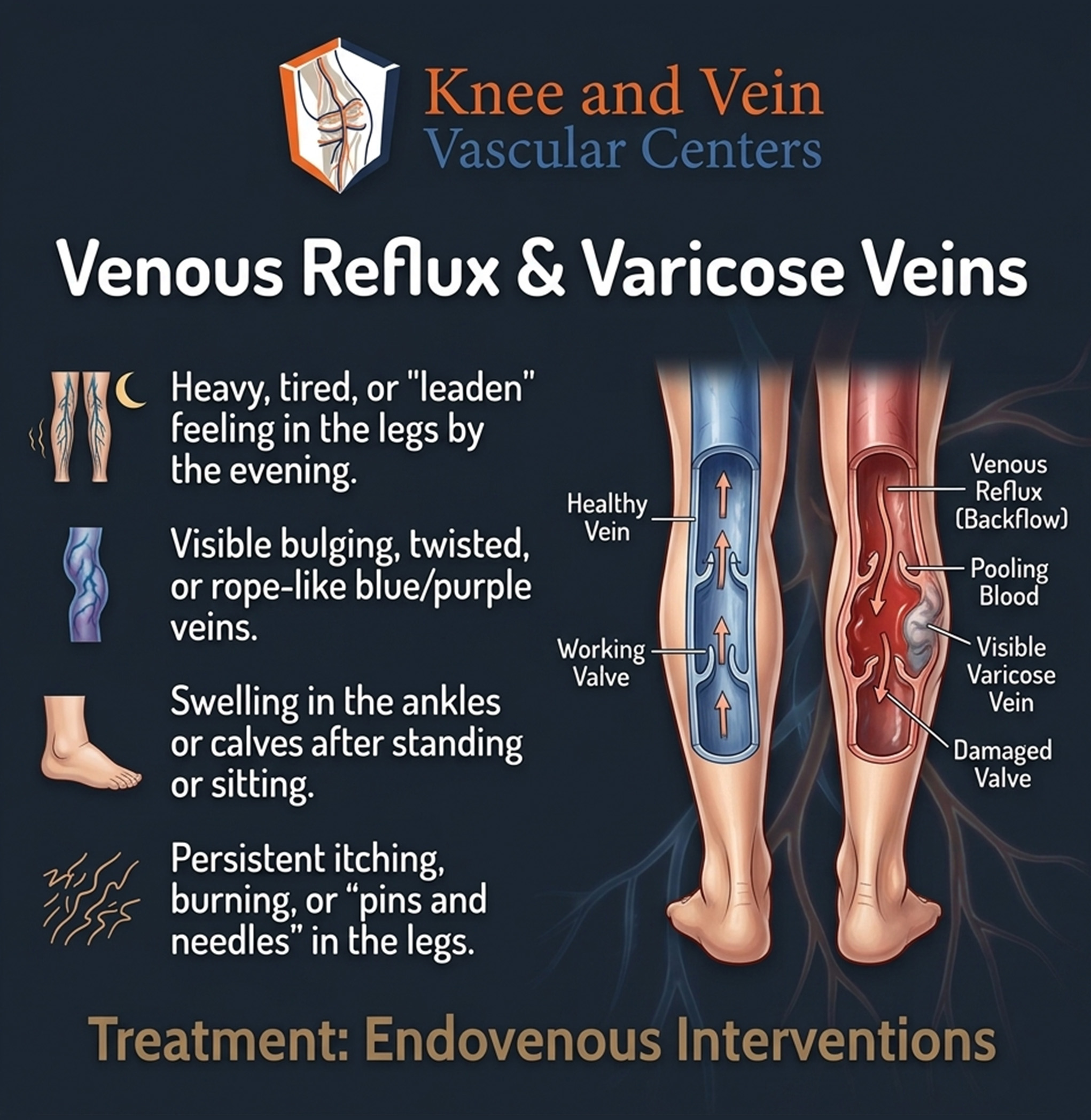
Understanding Varicose Veins
What are Varicose Veins?
Types of Visible Veins:
- Spider veins: Tiny red, blue, or purple web-like veins
- Reticular veins: Slightly larger bluish-green veins
- Varicose veins: Bulging veins 3 mm or more, twisted or rope-like
Your Symptoms Are Real and Treatable
- Aching, throbbing, or heaviness in the legs
- Fatigue, especially after standing
- Swelling of ankles and lower legs
- Burning, itching, or tenderness along veins
- Cramping or restless legs at night
- Skin changes (discoloration, dryness, thickening)
Why Varicose Veins Develop:
- Genetics (family history)
- Age (vein walls and valves weaken)
- Female sex and hormonal changes
- Pregnancy
- Obesity or prolonged standing/sitting
- Previous blood clots (DVT)
CEAP Classification:
Treatment Options for Varicose Veins
Conservative Treatments:
- Compression stockings to improve blood flow
- Leg elevation multiple times per day
- Walking and calf exercises
- Weight management and lifestyle adjustments
Minimally Invasive Procedures:
- Thermal closure (laser or radiofrequency)
- Sclerotherapy (liquid or foam)
- Medical adhesive/vein glue
- PDE5 inhibitors (tadalafil): Helps urinary symptoms and sexual function
What to Expect during Treatment
Evaluation & Planning:
- Review of symptoms and medical history
- Physical exam of legs while standing
- Venous ultrasound to assess reflux and vein anatomy
- Discussion of treatment options, including insurance coverage and self-pay options
Treatment Procedures:
- Thermal closure: Laser or radiofrequency energy closes diseased veins
- Sclerotherapy: Injection to collapse veins
- Vein glue: Seals the vein without compression
Recovery:
- Most patients walk immediately after procedures
- Return to normal activities in 1-2 days
- Compression stockings for 1-2 weeks as directed
Important Notes:
- Symptoms like pain, heaviness, and swelling are not normal and are treatable
- Early treatment can prevent progression to more serious complications
- Repeat treatments may be needed if new veins develop
Am I a Candidate? | Schedule a Consultation
- Have aching, heaviness, swelling, or pain in your legs
- Notice skin changes or bulging veins
- Have tried conservative treatments without relief
- Want minimally invasive treatment while avoiding surgery
Next Steps:
- Don’t ignore leg pain, heaviness, or swelling
- Schedule a consultation with a vein specialist
- Get a venous ultrasound to evaluate reflux and anatomy
- Discuss treatment options and insurance requirements
- Start conservative measures while awaiting evaluation
FAQS
BPH, or enlarged prostate, is a non-cancerous growth of the prostate gland that occurs as men age. The prostate surrounds the urethra, and when it enlarges, it can squeeze the urethra and cause urinary problems.
The exact cause of BPH is not fully understood, but it is related to hormonal changes that occur with aging. Risk factors include:
- Age (risk increases significantly after age 50)
- Family history of BPH
- Obesity
- Diabetes and heart disease
- Lack of physical activity
Your doctor will use several tools to assess the severity of your BPH:
International Prostate Symptom Score (IPSS): A questionnaire that measures your urinary symptoms on a scale of 0-35:
- Mild symptoms: 0-7 points
- Moderate symptoms: 8-19 points
- Severe symptoms: 20-35 points
Quality of Life (QoL) Score: Measures how much your symptoms bother you on a scale of 0-6
Peak Urinary Flow Rate (Qmax): Measures how fast you can urinate (normal is >15 mL/second)
Postvoid Residual (PVR): Measures how much urine remains in your bladder after urinating
Prostate Volume: Measured by ultrasound or MRI (normal prostate is about 20-30 grams)
Your doctor will use several tools to assess the severity of your BPH:
International Prostate Symptom Score (IPSS): A questionnaire that measures your urinary symptoms on a scale of 0-35:
- Mild symptoms: 0-7 points
- Moderate symptoms: 8-19 points
- Severe symptoms: 20-35 points
Quality of Life (QoL) Score: Measures how much your symptoms bother you on a scale of 0-6
Peak Urinary Flow Rate (Qmax): Measures how fast you can urinate (normal is >15 mL/second)
Postvoid Residual (PVR): Measures how much urine remains in your bladder after urinating
Prostate Volume: Measured by ultrasound or MRI (normal prostate is about 20-30 grams)
- By age 60, about 50% of men have BPH
- By age 85, approximately 90% of men are affected
- BPH is not cancer and does not increase cancer risk, but it can significantly impact quality of life
TESTIMONIALS