Understanding Enlarged Prostate (BPH) and Your Treatment Options
Ready to take the next step?
Hear from Dr. Costantino
Understanding BPH & Your Symptoms
What is Benign Prostatic Hyperplasia (BPH)?
How Common Is BPH?
- By age 60, about 50% of men have BPH
- By age 85, approximately 90% of men are affected
- BPH is not cancer and does not increase cancer risk, but it can significantly impact quality of life
Symptoms of BPH (Lower Urinary Tract Symptoms – LUTS)
Voiding (Emptying) Symptoms:
- Weak or slow urinary stream
- Difficulty starting urination (hesitancy)
- Straining to urinate
- Intermittent stream (stopping and starting)
- Dribbling at the end of urination
- Feeling of incomplete bladder emptying
Storage (Filling) Symptoms:
- Frequent urination (more than 8 times/day)
- Urgent need to urinate
- Waking at night to urinate (nocturia)
- Urinary leakage (incontinence)
Severe Complications (if untreated):
- Urinary retention (inability to urinate)
- Urinary tract infections
- Bladder stones
- Kidney damage
What Causes BPH?
- Age (risk rises after 50)
- Family history of BPH
- Obesity, diabetes, heart disease
- Lack of physical activity
- Hormonal changes
Measuring BPH Severity:
- IPSS Score: 0–7 mild, 8–19 moderate, 20–35 severe
- Quality of Life (QoL) Score: 0–6 scale of bother
- Peak Urinary Flow Rate (Qmax): Normal >15 mL/sec
- Post-void Residual (PVR): Measures urine left in bladder
- Prostate Volume: Ultrasound or MRI (normal ~20–30 grams)
Treatment Options for BPH
Conservative Measures (First Step):
- Watchful waiting for mild symptoms
- Lifestyle changes: limit fluids at night, reduce caffeine/alcohol, avoid medications that worsen symptoms
Medications:
- Alpha-blockers: Relax muscles in prostate/bladder neck for quick relief (days–weeks)
- 5-alpha reductase inhibitors: Shrink prostate over months; best for larger prostates (>40 g)
- Combination therapy: Can improve results for larger prostates
- PDE5 inhibitors (tadalafil): Helps urinary symptoms and sexual function
Surgical & Minimally Invasive Options:
- TURP: Gold standard surgery, effective but longer recovery, higher risk of retrograde ejaculation (65-75%)
- Laser options (HoLEP, GreenLight PVP): Less bleeding, effective for larger prostates
- Simple prostatectomy: Major surgery for very large prostates (>80-100 g)
Minimally Invasive Therapies (MIST):
- UroLift: Implants push prostate tissue away; preserves sexual function
- Rezum: Steam therapy; office-based, short recovery
- Aquablation: Water-jet removal of prostate tissue
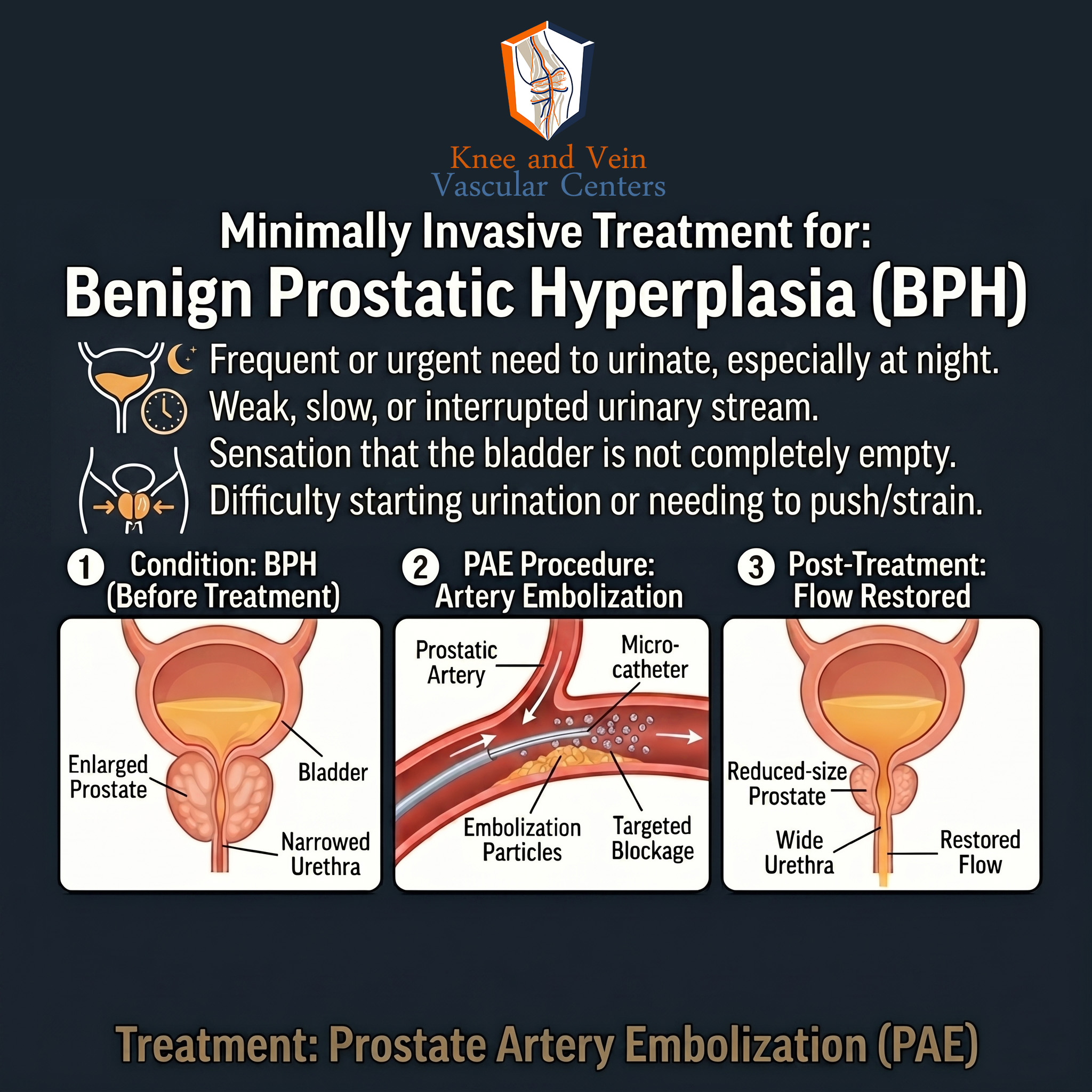
Prostate Artery Embolization (PAE):
- Office-based, minimally invasive procedure
- Shrinks prostate by blocking blood flow, relieving urinary symptoms
- Preserves sexual function and avoids catheter or general anesthesia
What to Expect with PAE
During the Procedure:
- Catheter inserted via wrist or groin under local anesthesia
- X-ray guidance to inject tiny microspheres into prostate arteries
- Usually treats both sides in 1-2 hours
- Recovery: monitored 1–2 hours, most go home same day
Post-Procedure Recovery:
- Mild pelvic discomfort, urinary urgency/frequency (post-embolization syndrome)
- Temporary dysuria, hematuria, or bruising at catheter site
- Most return to normal activities in 3–5 days
- Follow-up visits at 1, 6, and 12 months to track improvement
Effectiveness:
- Symptom improvement in 87–94% of patients
- IPSS decreases 50–70%, QoL improves 50–65%
- Peak urinary flow increases 50–100%, prostate volume decreases 25–30%
- Many stop BPH medications at 1 year
Durability & Reintervention:
- Benefits maintained 5-7 years
- 16–20% may need a second procedure within 7 years
- Surgical options remain available if PAE is not fully effective
Safety & Advantages:
- Rare major complications (<1%)
- Preserves ejaculatory and erectile function
- Avoids urinary incontinence
- Outpatient procedure; no catheter needed in most cases
Am I a Candidate? / Next Steps
Good Candidates for PAE:
- Moderate-to-severe BPH symptoms
- Tried medications with inadequate relief or intolerable side effects
- Prefer outpatient procedure with rapid recovery
- Want to preserve sexual function
- Poor surgical candidates due to age, medical conditions, or anticoagulation
Next Steps:
- Discuss your symptoms with your urologist or primary care doctor
- Get imaging to assess prostate size and suitability for PAE
- Explore conservative measures while evaluating procedural options
- Decide on a personalized treatment plan balancing safety, effectiveness, and lifestyle
FAQS
BPH, or enlarged prostate, is a non-cancerous growth of the prostate gland that occurs as men age. The prostate surrounds the urethra, and when it enlarges, it can squeeze the urethra and cause urinary problems.
The exact cause of BPH is not fully understood, but it is related to hormonal changes that occur with aging. Risk factors include:
- Age (risk increases significantly after age 50)
- Family history of BPH
- Obesity
- Diabetes and heart disease
- Lack of physical activity
Your doctor will use several tools to assess the severity of your BPH:
International Prostate Symptom Score (IPSS): A questionnaire that measures your urinary symptoms on a scale of 0-35:
- Mild symptoms: 0-7 points
- Moderate symptoms: 8-19 points
- Severe symptoms: 20-35 points
Quality of Life (QoL) Score: Measures how much your symptoms bother you on a scale of 0-6
Peak Urinary Flow Rate (Qmax): Measures how fast you can urinate (normal is >15 mL/second)
Postvoid Residual (PVR): Measures how much urine remains in your bladder after urinating
Prostate Volume: Measured by ultrasound or MRI (normal prostate is about 20-30 grams)
Your doctor will use several tools to assess the severity of your BPH:
International Prostate Symptom Score (IPSS): A questionnaire that measures your urinary symptoms on a scale of 0-35:
- Mild symptoms: 0-7 points
- Moderate symptoms: 8-19 points
- Severe symptoms: 20-35 points
Quality of Life (QoL) Score: Measures how much your symptoms bother you on a scale of 0-6
Peak Urinary Flow Rate (Qmax): Measures how fast you can urinate (normal is >15 mL/second)
Postvoid Residual (PVR): Measures how much urine remains in your bladder after urinating
Prostate Volume: Measured by ultrasound or MRI (normal prostate is about 20-30 grams)
- By age 60, about 50% of men have BPH
- By age 85, approximately 90% of men are affected
- BPH is not cancer and does not increase cancer risk, but it can significantly impact quality of life
TESTIMONIALS